In our first conversations about what would one day become Relationship-Based Care (RBC), we talked about what it would take for people in health care organizations to work together more collaboratively and with a higher degree of coordination of efforts, in order to more consistently provide safe, quality care for patients and families. These conversations soon expanded to include ideas about how a unit or department’s structures and processes could be refined to safeguard and perhaps even actively support the clinician-patient relationship. Relationship-Based Care is not unusual in its focus on relationships. It’s unusual because it is an operational framework that helps organizations do everything necessary to point all of its people, structures, and processes toward creating the best possible experience for patients, families, and all who work in health care.
It is often said that RBC works from the inside-out, meaning it appeals to and optimizes the very best of what already exists in people. It is common to hear comments like this one, from an RBC implementation leader: “RBC isn’t what we do; it’s who we are.” Because the transformation to a Relationship-Based Care culture is so deeply personal for so many people, it can become deeply rooted in the organization. In fact, relationship based healing cultures are designed to be so pervasively embodied within your organization that it becomes permanent.
What is Relationship-Based Care?

Relationship-Based Care is an organizational model for transforming health care into an enduring culture of extraordinary care.
The eight dimensions of the relationship based care model are:
- Healing culture
- Patients & families
- Leadership
- Teamwork
- Interprofessional practice
- Care delivery
- System design, and
- Evidence
Each of these dimensions must be carefully addressed if organizational excellence and widespread change in any health care environment are to be both systemic and sustainable. Here are the dimensions with brief descriptions:
Healing Culture
A healing culture holds all people—consumers of care and providers of care alike—with compassion, respect, and dignity. All are supported in learning and reaching their full potential, and each team member’s ability is valued for their contribution to the health and healing of patients. Consistent, high quality therapeutic relationships and a calming physical environment are core components of healing cultures.
Patient & Family at the Center of Everything

Structures, processes, and relationships are developed to aid each caregiver’s ability to provide attuned, compassionate, family centered, high quality care. Systems and services align with patient and family needs and priorities. Care is grounded in deep knowledge about the human response to illness and the power of therapeutic connection.
Leadership
Leaders cultivate a shared vision, inspire and model healthy relationships, and empower the people closest to the work to continuously improve their own structures, processes, and relationships. Leaders hold the wellbeing of patients, families, and staff members as their highest priority.
Teamwork
Teamwork requires people from all disciplines and departments to define and embrace a shared purpose and work together with trust and mutual respect. Consistent and visible teamwork is essential to the provision of high quality, safe care.
Interprofessional Practice
All clinical professionals are respected and valued for their unique expertise and full scope of practice. Clinical practice is grounded in research, professional standards, and ethics. Diverse perspectives are essential to effective collaboration and optimal patient care and outcomes.
Care Delivery System
A patient care delivery system is a structure for organizing care. In an RBC organization, care is designed to allow clinicians to accept individual ownership for the patient-clinician relationship and form a therapeutic relationship with the patient and family. In an RBC culture, fragmented processes are replaced with processes that enable continuity of relationships and smooth transitions across the continuum of care.
System Design
Structures, processes, and people are all consciously pointed toward bringing clinical quality, relational excellence, safety, effectiveness, and efficiency to patient care and the work environment.
Evidence
Desired outcomes are identified and shared as evidence of achievement of the organization’s mission and vision. Clinical and leadership practices are supported by current evidence and continuous learning and development. Celebration of the successful movement toward reaching goals helps build commitment and unity within an organization.
Given the realities of the ever-increasing complexity of health care, how can an organization advance cultures that are consistently healing for patients, families, and all the people working in health care? We have seen organizations throughout the world move steadily toward creating and sustaining just such cultures. It is always an ongoing process, with progress some days measured in inches rather than miles, but the successes we have seen and continue to see inspire us every day.
The Three Key Relationships

After decades of guiding Relationship-Based Care implementations across the world, we know that the content that consistently elicits the most excitement is what we call “the three key relationships”: relationship with self, relationship with colleagues, and relationship with patients and families.
Relationship with Self
To stay healthy and be emotionally available to others, caregivers pay attention to their own energy levels, are self-aware and mindful as they interact with patients, families, and each other, and practice self-care for body, mind, and spirit.
Relationship with Colleagues
Healthy interpersonal relationships and purposeful collaboration among team members positively impact the work culture and the patient experience All team members model mutual respect, trust, open and honest communication, and consistent, visible support promoting a healthy environment.
Relationship with Patient and Families

In RBC cultures, patients are seen, heard, and cared for as distinct individuals. Care and service are designed to prevent unnecessary suffering due to delays, physical or emotional discomfort, and lack of information about what is happening. Patients are included as members of the health care team.
The order in which we talk about the three relationships is deliberate. Long and Smith put it this way, “As leaders, it is tempting to put nearly all of our attention on the desired outcome of exemplary patient care, as opposed to thinking through how fundamental the self-care of everyone in the organization is to that vital outcome.”[1]
Whether as a patient or a care provider, we experience the essence of care in the moment when one human being connects to another. When compassion and care are conveyed through touch, an attuned act, through competent clinical interventions, or through listening and seeking to understand the other’s experience, a healing relationship is advanced. This is the heart of Relationship-Based Care.
The Culture Transformation Mindset

Author and organizational consultant, Simon Sinek, in his book The Infinite Game, gives voice to something those embarking on the transformation to a Relationship-Based Care culture know well: “In infinite games, like business or politics or life itself, the players come and go, the rules are changeable, and there is no defined endpoint….There are no winners or losers…; there is only ahead and behind.”[4] In games with no defined endpoint, where players leave and new players can enter at any time, winning is not about crossing a defined finish line at a set point in time. Instead, it’s about persisting. It’s about moving forward for the foreseeable future in direct service to a just cause.
Client organizations who have RBC enculturated reported that they were grateful to have it as a foundation as they navigated the disruption of the pandemic. The framework kept them focused and resources aligned. They maintained a clear understanding on the vital importance of caring for individuals and teams through the surges of the pandemic and the uncertainty that prevailed. Their leaders made sure their team members were heard, protected, supported, and prepared. Their team members felt seen and valued. There was a spirit of “being in this together.” The constancy of RBC principles and practices impacted their ability to sustain well-being and prevent turnover.
In the infinite game of health care, the equilibrium of your organization is likely to be shaken (if not shattered) by leadership turnover, mergers, epidemics, serious weather events, systemic changes in insurance or reimbursement models, and much more. Relationship-Based Care provides consistent coherence in a world that is ever changing.
Measurement is essential in health care. So, what do you think you would measure if you knew you were playing an infinite game? How focused would you be on moving three or four key measures one or two points? And if you were a member of the board of an organization that knew it was playing an infinite game, how would you measure the success of the organization? What kinds of things would you incentivize your CEO to do or not do? What would you measure if you were no longer focused on the basic concepts of winning or losing—if you were primarily focused on improving, learning, enduring, and embodying a noble and altruistic mission?
Relational and Clinical Competence
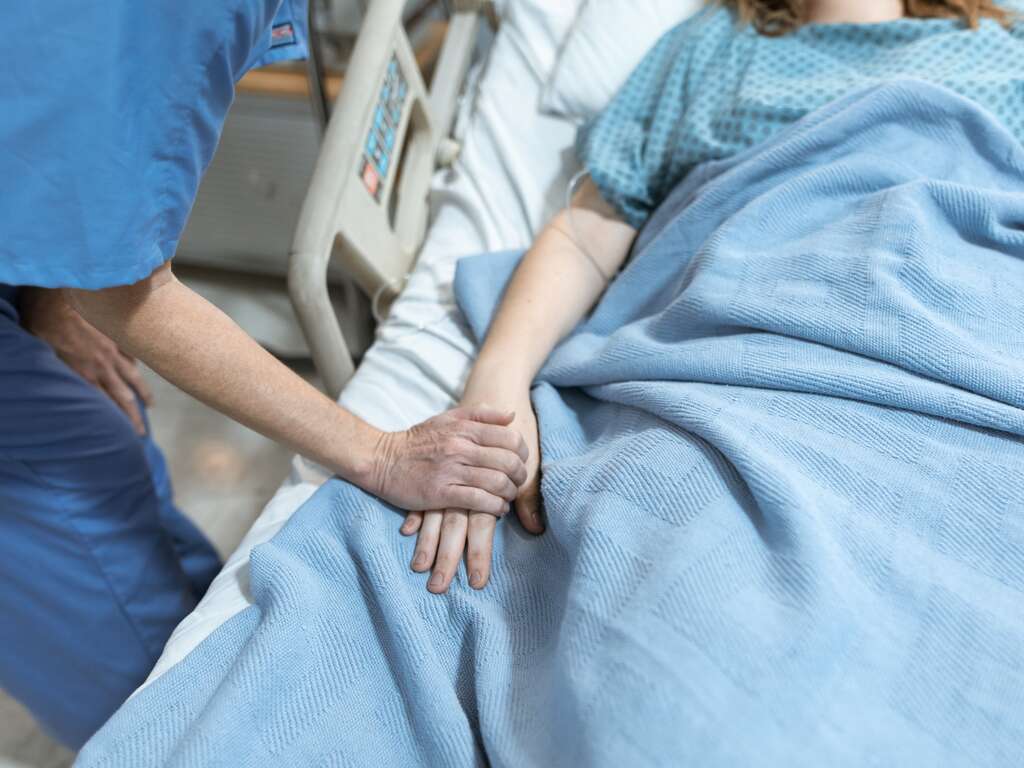
It is a given, in health care, that there will always be too many things to focus on. There are, and will always be, multiple initiatives in play in your organization. So, here is a bit of insight that may help you manage that reality: You cannot focus people on improving metrics in quality, safety, patient experience, employee and physician engagement, and the financial performance, and expect relationships to improve as a byproduct of that focus. But you can focus people on improving and nurturing relationships—one thing—and expect quality, safety, patient experience, employee and physician engagement, and the bottom line to improve.
As you embark on your culture transformation journey, it’s important to ask yourself this question: What do you want your legacy to be? When your time in the organization is done, will you and your team be the people who moved the dial on two or three key metrics? Or will you be the people who made it standard operating procedure in your organization for people to take care of themselves, to take care of each other, and to take ownership for and pride in their work? Will you be the people who elevate and honor the work of human caring and cultivate a team of health care professionals who are committed to the best possible care for every life they touch? You are already building your legacy, and it’s never too late to refine it.
MAGNET®, Magnet Recognition Program®, ANCC Magnet Recognition®, Journey to Magnet Excellence®, Pathway to Excellence® Program, Pathway to Excellence in Long Term Care®, Demographic Data Collection Tool®, DDCT®, Practice Transition Accreditation Program® (PTAP) are registered trademarks of the American Nurses Credentialing Center (ANCC). The products and services of Creative Health Care Management are neither sponsored nor endorsed by ANCC. All rights reserved. The content presented in here is the expressed opinion of the author/presenter and not that of the American Nurses Credentialing Center (ANCC).
References
[1] Long, B, & Smith, R. (2017). Attuning, wondering, following, and holding as self-care (p. 36). In M. Koloroutis, & D. Abelson (Eds.). Advancing relationship-based cultures. Minneapolis, MN: Creative Health Care Management.
[2] Adapted from Koloroutis, M., Felgen, J., Person, C., & Wessel, S. (2007). The why of Relationship-Based Care: A vision emerges through want of something more. In M. Koloroutis, J. Felgen, C. Person, & S. Wessel (Eds.). Relationship-Based Care field guide: Visions strategies tools and exemplars for transforming practice (pp. 14-18). Minneapolis, MN: Creative Health Care Management.
[4] Sinek, S. (2019). The infinite game. New York: Penguin Random House, LLC.
Mary has spent more than four decades advancing relationship-based cultures in health care organizations. She partners with clients to identify and maximize the strengths and capacities of teams and whole systems. The results speak for themselves: measurable improvement including widespread alignment with core values and principles.


