The COVID-19 pandemic brought to the forefront longstanding issues in the health care system. A strained and underfunded system put the health of both patients and caregivers at risk jeopardizing true health care heroes.
Employee engagement in the healthcare industry is crucial in maintaining high-quality care and reducing costs. In addition, high employee turnover and job satisfaction negatively impact patient safety and health outcomes.
Many healthcare organizations today are facing high employee turnover rates and heavy competition for top candidates. As a result, retention strategies are essential. Recognition programs can be an excellent way to retain top performers and foster a sense of community in the workplace. If done correctly, recognition can be a powerful retention strategy.
A leader’s personal characteristics also influence their success. They must be a visionary who can set ambitious goals and lead a team toward them. A visionary leader demonstrates respect for others and seeks out their input.
Health care heroes are also be role models for the culture of an organization. A healthcare leader’s mentoring role can have a positive impact on a healthcare student’s professional development. By sharing their insights and skills with a student, a healthcare leader can encourage and motivate a young professional and help him or her set career goals.
Frontline Health Care Workers
The COVID-19 pandemic is a public health issue with significant ramifications for frontline health care workers.
According to a recent online survey by Mental Health America, 93% of health care workers reported high levels of stress, exhaustion, frustration, and anxiety, which may contribute to their poor physical and mental health. Moreover, more than half reported worrying about exposing their children or loved ones, while 47% expressed concern about their spouse or partner.
The COVID-19 mental health burden for our frontline care heroes is especially high among younger workers, with one in eight reporting a negative impact on their healthiest life.
More than half of this population is under thirty, and many younger workers help with patient care. The COVID-19 pandemic has also caused the deaths of many frontline health care support, affecting their physical and mental well-being.
Nursing Professionals
Nurses are among the many health care heroes who have worked tirelessly during the current pandemic. They are typically the first person to see a patient. Nursing is one of the most sought-after and rewarding professions, but it comes with challenges.
Nurses are often overworked and understaffed, leading to feelings of frustration. This frustration can lead to burnout, which is an extreme form of job-related stress that can have serious consequences for both nurses and patient care.
Nurses who have experienced burnout understand the emotional strain was from the chronic stress of a challenging, high intensity work environment. Burnout can be attributed to emotional exhaustion, an unpleasant work environment, or job dissatisfaction often related to not feeling heard or valued.
The Covid 19 Pandemic

With Covid 19 the patient mortality was something most nurses could not fathom seeing in their lifetime. To experience burnout while seeing so many suffering was a double edge sword, how could a nurse leave during the pandemic.
For some just entering nursing, seeing the devastation renewed their commitment. Veteran nurses seemed to have superpowers. Together we watched the nursing community pull together and it was breathtaking.
Sources of Stress for Frontline Doctors
The recent outbreak of the Coronavirus 2019 has raised the profile of psychological stress in doctors and nurses. This new virus has spread across the world, and has been linked with higher levels of somatization and terror among our supporting front line.
In Wuhan, China, nearly one-third of frontline healthcare workers reported high levels of anxiety. Understanding the sources of stress in frontline healthcare workers is vital for improving their psychological health.
Mental Health
It is vital to monitor the mental health of all health care staff during outbreaks like COVID-19. When addressing crucial issues that effect the lives in our society and country, such as preventing the spread of the virus, we must also address the mental health among our health care heroes.
Ensuring coverage and empowering our health care heroes is a necessary component of maintaining essential health services during any outbreak like COVID-19. It is relevant to expect and consider the data and statistics for broader implications of a COVID-19 pandemic to ensure the safety of all.
The outbreak of COVID-19 led to a significant increase in the number of patients and health care staff with COVID-19. Although this outbreak has resulted in a higher level of stress in patients, few studies have examined the impacts on the focus of our health care heroes. It has also been shown that healthcare workers who experience COVID-19 exposure and the symptoms of acute stress are at a significantly higher risk for chronic illness.
The Impact of Public Attitudes in Support of Mental Health for Frontline Workers in Hospitals
Despite widespread concern about COVID-19, there is a growing body of evidence showing that frontline workers in hospitals are at risk of significant psychological distress.
The healthcare workforce is suffering from increased anxiety, insomnia, and depression. The reasons why are inconsistent, but it is clear that frontline workers in hospitals are exposed to increased risks with little response or support for mental health access in every city in the country. This is particularly true of those who are directly exposed to COVID-19.
Public attitudes about vaccines play a critical role in healthcare worker safety, and are likely to affect the effectiveness of various interventions. In the case of COVID-19, four-fifths of frontline workers in hospitals have received the two doses of the vaccine, while one-quarter have not scheduled their vaccination.
Treatment for Mental Illness
Currently, less than half of our society receives treatment for mental illness. The causes are many. Lack of sufficient access to mental health providers in each city and their communities, a fragmented healthcare system, and a culture that shames seeking care. Further, mental illness is also stigmatized in the United States, which further impedes access to treat those who seek their healthiest life and mental health care.
How do Health Care Workers Stay Protected?
At the beginning of the pandemic it was a major concern that staff would contract the Covid 19 virus from being exposed on a frequent basis. This was due to the fact that so many hospitals, doctor’s offices, and other healthcare facilities needed protective equipment. It was hard to find, and sometimes almost impossible to get.
Personal Protective Equipment
There were limited resources for personal protective equipment (PPE) and some hospitals struggled to supply it for their staff.
Personal protective equipment, also known as “PPE”, is equipment worn to minimize exposure to hazards that cause serious illnesses or workplace injuries. These illnesses and injuries may result from contact with physical, mechanical, chemical, radiological, electrical, or other workplace hazards.
Support for Frontline Health Care Workers
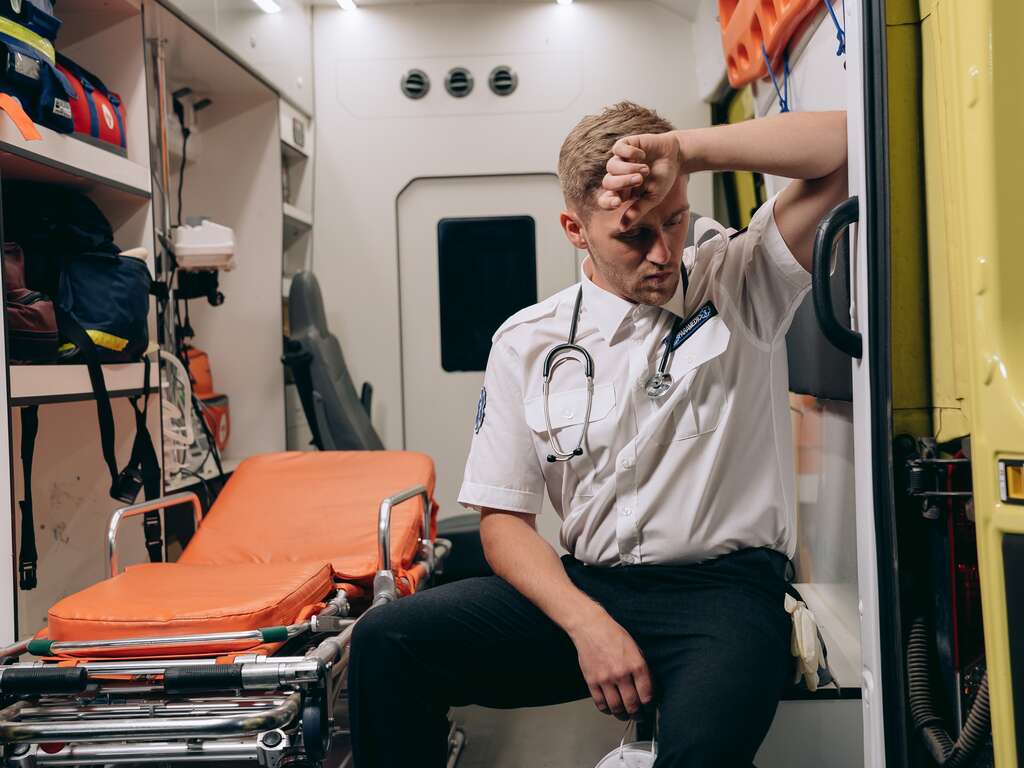
Despite increasing demands, health care workers are still under tremendous stress. In a volatile environment, healthcare workers face heightened risk of infection, as well as insufficient preparation for emergencies.
Additionally, many frontline workers are forced into roles they do not know or situations where they lack social support. Below are some ways to support frontline health care workers.
Frontline Health Workers Coalition
The Frontline Health Workers Coalition is a global coalition of public and private organizations that advocate for increased strategic investment in frontline health workers, particularly in low and middle-income countries.
The organization also serves as a watchdog function for multilateral institutions and the United States government, and partners with health workers, unions, and other advocates around the world. Their mission is to make sure every community has access to basic health care services.
Supportive Environment
Leaders of frontline health care workers must create a supportive environment. They must acknowledge that their team members face extra stress and that their own needs are equally important.
As a result, they must not overburden frontline workers. Instead, they should be willing to share their burdens and provide enough space to work through the problems that arise. It is important to remember that healthcare workers need their own space and time, too.
Creative Health Care Management
CHCM provides consultation services, educational programs, and products to executives, leaders, and all clinical and support staff members. Our mission is to partner with clients to cultivate sustainable improvements.
Our consultants help you leverage the power of relationships across organizations, resulting in everyday innovation and performance improvement. We help you create healing environments where employees are empowered to take ownership of their work. Patients and families truly feel held at the center of care.

Nursing Retention
The process of retaining nurses in hospital settings or medical practices is known as “Nursing Retention”.

Physician Resilience
Physician resilience is best described when doctors in private practice or working in a hospital setting is able to maintain both emotional health and performance when demands and pressure are difficult.

Compassion Fatigue in Nursing
Compassion fatigue is the result of prolonged exposure to emotional distress or trauma without adequate emotional processing.
It affects people who work with traumatized populations or in other high-stress environments and manifests as feelings of hopelessness, powerlessness, disconnection from others and oneself, depression, anxiety, anger, and irritability.

Nurse Burnout
Nursing burnout is a condition of mental and physical exhaustion that can affect nurses caused by stressful working environments, working long hours, too many patients to care for, and not getting enough rest. It can also lead to a decrease in the quality of the care given by nurses.
Since the emergence of Covid-19, the nursing workforce burnout rate has been steady at around 50% among nurses while turnover rates have increased to between 20% and 30%. Prior to the pandemic, about one-third of nurses reported burnout, and turnover was about 17% per year.


